Non-steroidal anti-inflammatory treatment, therapy, and even stem cell injections are common solutions for knee pain when non-surgically possible. As a substitute for surgery, these options may ease your pain and ensure your overall health without the stress and recovery. However, surgery is occasionally necessary.
Some patients with knee discomfort may benefit from complete knee replacement surgery. For good results and a faster recovery time than in the past, technological growth has made this treatment less daunting. It is now possible for surgeons to do robotic-assisted complete knee replacements, leading to better surgical results for you.
Developments in Total Knee Replacement from the Past to The Present Day
Compared to its early days, replacement knee surgery has made important progress. More than three million knee replacements are expected to be undertaken by 2030, an increase in operations performed annually. The use of robotic arms for precise surgery had evolved better from the days when iron was employed as a joint substitute.
The very first operation to completely replace a patient’s knee joint took place in 1968. However, the manufacture of the complete knee arthroplasty didn’t begin until the early 1860s, when a German surgeon named Themistocles Gluck surgically inserted an iron hinge joint for the first time. This was the beginning of the procedure. The Walldius hinge joint did not make its debut until 1951 and was first fabricated from acrylic. In 1958, the material element was changed to cobalt and chrome.
In the 1960s, John Charnley created metal-on-polyethylene total hip arthroplasty, which influenced parts of total knee replacement. Frank Gunston invented an unfastened knee that substituted both the medial and lateral portions of the joint using independent condylar elements.
The approach was employed throughout the 1970s as component materials, shape, and fastening features steadily improved. Since then, there have been attempts to refine sizing, improve instrumentation, bigger range, and the possibility of patella-femoral replacement. Nowadays, technology has become a big element of the process in which knee arthroplasty is performed.
Robotic-Arm Assisted Surgery (RAS) is a specialty in Integrated Orthopedics. In 2004, Rony Abovitz, Maurice Ferre M.D., and other Z-KAT, Inc. team members launched Mako Surgical. Their Whole Arm Manipulator, first developed at MIT and afterwards at Barrett Technology, was a unique haptic robotic device for medical purposes that they worked on together.
What is Traditional Knee Surgery?
The affected or damaged knee surfaces are replaced using an orthopedic process known as traditional knee replacement. To help patients return to their regular lives, a “prosthesis” or implant can be used to replace the damaged surfaces and relieve pain and improve movement.
A long, vertical incision in the center of the knee is used in the typical knee replacement procedure to get access to and see the joint. An example of this procedure is a noninvasive knee replacement. Shorter incisions and alternative techniques expose the joint to reduce postoperative pain and expedite healing.
Robot Assisted Knee Surgery
If you’re suffering from early to middle-stage knee arthritis, you may be a candidate for Mako knee replacement surgery. The Robotic Arm Interactive Orthopedic System is utilized to perform partial knee resurfacing.
The infected part of the knee is revived during the therapies, preserving the patient’s better and healthier bone and tissue. After that, an implant is placed inside the joint to restore the knee’s natural range of motion.
Benefits of Robotic Knee Surgery
Compared to the past age of knee surgeries, robot-assisted knee replacements make a main improvement in the field. Using pre-operative 3D imagery and research, surgeons can implant knee sections specifically tailored to each patient’s structure.
Robotic surgery is less invasive than traditional knee replacement, with minimally invasive incisions, less damage to closer bone and tissue, and bigger accuracy. With more accurate knee surgical treatment, new parts have less abrasive wear, reducing the need for further revision surgery.
Recovery Times After Robotic Surgery
The procedure itself will take around an hour. After the treatment, patients are allowed to walk, and within two weeks, most are back to their regular daily routines, including driving a vehicle. Mako techniques involve fewer soft tissue releases compared to standard non robotic methods. This results in reduced discomfort and a faster recovery time. Thanks to the Mako technology, you may walk more naturally and sooner, which allows your surgeon to align your joints properly.
When Compared to Traditional Open Surgery, Can Robotic Surgery Cause Greater Discomfort?
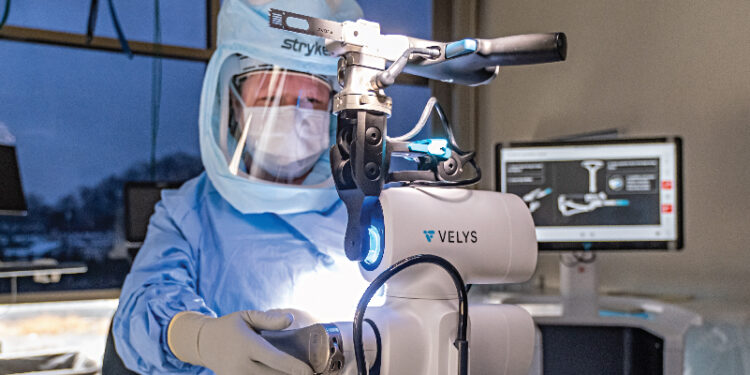
As a result of new pain control approaches and the Mako process itself, patients are experiencing less discomfort than in the past. Patients report less discomfort and faster recovery because of the surgery’s reduced invasiveness than traditional knee replacement, which causes less disruption to the bone and tissue around the incisions.
Qualified Candidates for the Knee Surgery
Those who need mako replacement surgery have significant joint discomfort or stiffness due to non-inflammatory degenerative joint illnesses such as osteoarthritis, post-traumatic arthritis (PTA), or avascular necrosis. Some people may discover that Mako is a viable choice if they’ve tried and failed with other approaches, such as braces, medicine, or joint fluid supplements.
Mako is not recommended for patients with certain infections, mental or neuromuscular disorders that would put them at unacceptable risk, prosthesis fixation failures because it would not work correctly, postoperative care complications in the past, or patients with weakened bone stock, skeletal immaturity, or severe joint instability.
Who Performs the Robot Assist Knee Surgery?
The surgeon uses a robotic arm to eliminate arthritic bone and cartilage throughout all procedures. In addition to adding visual signals, the surgeon may employ a virtual border throughout the procedure, making this a one-of-a-kind experience. Mako is a machine, not a doctor. While Mako knee replacement instruments have revolutionized the field of surgery, you will still need a reputable and well-respected surgeon who is educated in the Mako system. It is very important that you find an orthopedic surgeon who is licensed to perform this method, a good example would be Integrated Orthopedics in Scottsdale, AZ.
Cons of Knee Replacement with Robotic Assist
Mako has several drawbacks, just like any other surgical technique, including;
- Patients may be at greater risk of infection because of the longer surgical procedure required.
- Computers are only as good as their inputs, which holds for computer systems. The quality of the scans and their ability to work with Mako are important factors in determining the procedure’s success. Having the right expertise and All training ensures a successful surgical procedure and the best possible final result.
- Because it’s a novel technology, there’s no long-term evidence to support the claim that it improves implant function. Actual implants utilized already are typically proven and tested prosthesis.
In Summary

Robotic surgery has been shown to be superior to conventional knee replacement outcomes. Using robots to carry out procedures has been found to provide more accurate outcomes. More precise robotic assistance allows for less traumatic regions of bone and tissue, resulting in better outcomes.
 Hi Boox Popular Magazine 2024
Hi Boox Popular Magazine 2024



